Anesthesia Workforce Strategies: Flexibility, Feedback, and Scalable Staffing Models

It’s easy to measure workforce stability by what’s visible: staffed rooms, full schedules, and coverage in place. However, true workforce sustainability is driven by what’s happening behind the scenes, the strategies, support, and structure that allow organizations to maintain coverage consistently and scale it as demand shifts.
During Medicus’ ASA ADVANCE session, The Next Phase of Anesthesia Staffing: Smarter Models, Stronger Teams, healthcare leaders pointed to flexibility, feedback, and onboarding as important parts of sustaining an anesthesia program over time. Their perspectives offered a closer look at how workforce stability is supported as clinician expectations shift and care delivery continues to evolve.
 |
Mohammed Minhaj, MD, MBA, FASA, FACHEHarris Family Foundation Chair, Department of Anesthesiology, Critical Care and Pain Medicine, NorthShore, Swedish, and Northwest Community Hospitals |
 |
Matthew BelangerSystem Vice President, Surgical Services & Anesthesia at Endeavor Health |
 |
Francesco Sessa, MS, MBA, CRNAChief Nurse Anesthetist at Endeavor Health |
Understanding How Organizations Are Adapting to Workforce Expectations
To ground the discussion in current workforce realities, session attendees were asked how their anesthesia programs are adapting to the expectations of newer-generation clinicians.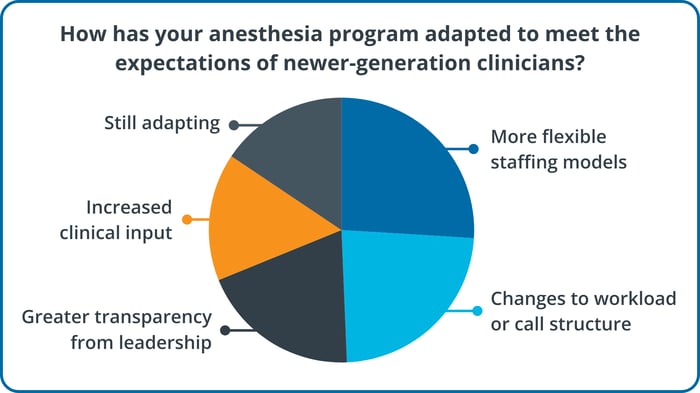
Taken together, the responses reflected several of the same themes that emerged throughout the discussion, particularly around flexibility, transparency, and clinician engagement.
Investing in Onboarding & Clinical Readiness for Long-Term Stability
During the panel, Dr. Minhaj cited workforce estimates suggesting it may take approximately 1.4 new-generation physicians to replace one boomer-generation physician. At Endeavor Health, that shift is showing up not only in recruitment but also in how new clinicians are prepared for practice.
Dr. Minhaj explained that care in community hospitals looks different from what it did 10 or 15 years ago. As more advanced procedures are being performed closer to home, clinicians entering those settings are expected to care for a broader range of patients and cases. In response, Endeavor Health has placed greater emphasis on helping new hires build confidence in that environment from the start.
“We have found that the onboard and the onramp time is a little bit longer,” Dr. Minhaj said. “We’ve got to invest more in terms of that period of time that we get them comfortable.”
In response, the department has taken a more structured approach to onboarding, including mini boot camps and dedicated time in subspecialty areas to help new hires build confidence in the types of cases they will encounter. Dr. Minhaj also pointed to the value of strengthening the broader support structure around the anesthesia team, including technician pipelines and educational programs that support long-term workforce development.
Leveraging Flexibility as a Recruitment & Retention Tool
As physician shortages persist, particularly in anesthesia, recruitment and retention remain central to staffing stability. At Endeavor Health, leaders are addressing this by building greater flexibility into the work environment, particularly around scheduling.
Sessa described a model that gives anesthesiologists and CRNAs greater control over how they structure their time through self-scheduling, varied shift options, and flexible FTE arrangements. Scheduling software supports that approach by giving providers visibility into staffing needs across more than 80 anesthetizing locations, allowing them to self-schedule within set blocks and adjust when coverage is already strong.
“This software and self-scheduling really help them feel like they have a lot of control over their schedule,” Sessa said. “And I really think that’s one of the reasons why we have some strong retention.”
In a highly competitive market like Chicago, where organizations often recruit from a limited pool of anesthesiologists and CRNAs, Sessa noted that flexibility, culture, and collaboration can be important differentiators.
Creating Feedback Loops to Implement & Sustain Change
As staffing models evolve, communication becomes just as critical as the changes themselves. Clear feedback and transparency are essential to sustaining progress, especially when staffing decisions impact teams across the perioperative environment.
Belanger explained that as surgical growth and anesthesia staffing become more closely connected, communication needs to move beyond occasional updates. Regular conversations about strategy, performance, and operational constraints help ensure that clinicians understand the reasoning behind changes and how those decisions support broader organizational goals.
“When there’s regular cadence to that, and it’s not just pulling people together to announce some big thing, it’s creating that particular connection that allows people to be less reactive, and help create space for strategizing,” Belanger said.
Sessa described a similar emphasis on feedback within the department. Alongside recurring meetings and leadership updates, his team uses a tool that allows providers to quickly signal how their day is going, giving leaders real-time visibility into operational challenges. That daily feedback creates a continuous connection between leadership decisions and frontline experience, helping teams adapt more quickly when adjustments are needed.
The Importance of Having a Flexible Interim Staffing Partner
As clinical staffing shortages persist, there is rarely a single solution that works for every organization. Strategies that improve stability in one system may look very different in another. What often makes the difference is whether leaders have the support in place to test and implement those ideas without being pulled away from the broader work of leading their departments.
During the panel discussion, leaders described how interim staffing support through the Medicus Transition Program helped stabilize anesthesia services during a period of change. That support created more space for leadership to focus on broader priorities, including culture, retention, onboarding, and implementation of a care team model. For organizations navigating similar challenges, that kind of support can play an important role in creating the operational space needed to implement change more effectively.
Interested in learning more about the Medicus Transition Program? Complete the short form below to connect with a member of the Medicus team.


